TMS therapy for PTSD can provide meaningful, lasting relief for many trauma survivors – especially those who haven’t responded well to medication or talk therapy. Research shows that repetitive transcranial magnetic stimulation targets the brain circuits disrupted by trauma, helping reduce flashbacks, hyperarousal, and emotional numbness. While results vary, clinical studies suggest improvements can persist for months – and in some cases, well beyond a year.
Trauma leaves a mark – not just emotionally, but neurologically. For millions of people with PTSD, that mark shapes every day: broken sleep, constant low-level anxiety, avoidance of ordinary places. Standard treatments help many, but not everyone. A real portion of people either don’t respond adequately or can’t tolerate medication long-term.
That’s where TMS (Transcranial Magnetic Stimulation) comes in – a non-invasive brain stimulation technique gaining ground as a legitimate alternative for treatment-resistant cases. No sedation, minimal side effects, and growing clinical evidence behind it.
What Is PTSD and How Does It Affect Daily Life?
Before looking at treatment options, it helps to understand what PTSD actually is – and why it can be so stubborn to treat.
Understanding the Condition
Post-traumatic stress disorder develops after exposure to a traumatic event – combat, assault, accidents, or childhood abuse. Not everyone who goes through trauma develops PTSD, but for those who do, the condition carries a lifetime prevalence of 7–12% in the U.S. and can become deeply disabling.
PTSD symptoms fall into four main categories:
- Re-experiencing – intrusive memories, nightmares, and flashbacks that feel as real as the original event
- Avoidance – steering clear of people, places, or topics that trigger distress
- Negative mood and thinking – persistent guilt, shame, or emotional numbness
- Hyperarousal –constant edginess, poor sleep, and an exaggerated startle response
These symptoms need to be present for at least a month to qualify as PTSD – and without treatment, they often stick around for years.
The Ripple Effects on Everyday Life
PTSD doesn’t stay in one lane. Relationships fray from emotional withdrawal. Work suffers when focus is constantly broken. Physical health takes a hit too – the condition is linked to higher rates of chronic pain, heart problems, and digestive issues.
For those dealing with TMS for complex PTSD, where trauma was prolonged or started in childhood, the picture is even more complicated. Complex PTSD disrupts identity and emotional regulation at a deeper level, which is part of why standard treatments often fall short.
Traditional Treatments for PTSD: What Works and What Doesn’t
Several established approaches exist – each with real strengths, but also gaps that leave some patients without adequate relief.
Common PTSD Therapies
The most widely used treatments for PTSD include:
- Cognitive Processing Therapy (CPT) – helps reframe distorted thoughts tied to the trauma
- Prolonged Exposure Therapy (PE) – gradually reduces fear by working through trauma-related memories
- EMDR – uses bilateral stimulation to help the brain process traumatic experiences differently
- Medication – SSRIs like sertraline and paroxetine are FDA-approved for PTSD and help stabilize mood
These work well for many people. But they don’t work for everyone.
Limitations of Traditional Treatments
A significant share of PTSD patients don’t respond well to first-line treatments – or they stop because the side effects or emotional demands become too much. Medication can take weeks to kick in, carries a long list of possible side effects, and doesn’t address the underlying neural patterns behind PTSD. Some people, especially survivors of chronic or early-life trauma, find that therapy alone simply isn’t enough.
That gap is a big reason why TMS treatment for PTSD has drawn growing interest from clinicians and researchers alike.
TMS Therapy for PTSD: How It Works
Understanding the mechanics of TMS helps explain why it can work when other treatments haven’t.
What Is TMS?
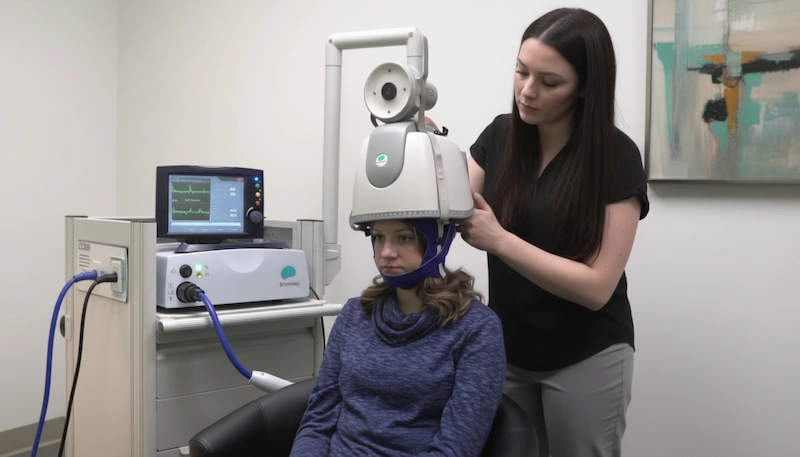
Transcranial Magnetic Stimulation uses focused magnetic pulses to stimulate specific brain regions. A coil placed on the scalp sends these pulses painlessly through the skull, modulating targeted neural circuits – no anesthesia, no downtime, and patients can drive themselves home after each session.
A typical TMS course runs five days a week over four to six weeks, with sessions lasting 20 to 45 minutes. Newer approaches, like deep TMS for PTSD, use specially designed H-coils that reach deeper brain structures – potentially more relevant for the entrenched patterns seen in PTSD.
How TMS Works for PTSD
PTSD throws several brain networks out of balance. The prefrontal cortex – which handles emotional regulation – tends to go quiet, while the amygdala, which drives fear responses, runs in overdrive. That imbalance makes it hard to switch off threat responses even in safe situations.
TMS targets this directly. Stimulating the dorsolateral prefrontal cortex, it helps restore balance between these regions. High-frequency pulses boost underactive areas; low-frequency ones calm overactive circuits. For many patients, the result is a noticeable drop in the hypervigilance and emotional reactivity that define PTSD.

How TMS Therapy for PTSD Helps in Trauma Healing
The evidence for TMS has built steadily over the past decade – enough that it’s moved well past “experimental” into genuinely recognized clinical territory.
TMS for PTSD: A Breakthrough in Treatment
A large multisite cohort study published in Brain Stimulation (2025), which tracked 756 veterans with PTSD and depression across multiple VA sites, found that TMS produced a roughly 19-point reduction in PTSD symptoms on the PCL-5 scale – statistically significant and clinically meaningful. Over 65% of participants showed meaningful improvement, and nearly half no longer met PTSD severity criteria by the end of treatment. Results held across three protocols, including deep TMS for PTSD.
That’s real-world data from a large patient population – not a tightly controlled lab setting.
| Treatment | Primary Mechanism | Effectiveness for PTSD | Side Effects | Accessibility |
| TMS Therapy | Brain stimulation via magnetic pulses | High, especially for resistant cases | Minimal (mild headache, scalp discomfort) | Outpatient; no downtime |
| SSRI Medication | Serotonin modulation | Moderate | Weight gain, sexual dysfunction, and insomnia | Highly prescribed |
| Prolonged Exposure | Trauma memory processing | Moderate to high | Requires a trained therapist | |
| EMDR | Bilateral stimulation + memory processing | Moderate to high | Emotional fatigue | Requires a trained therapist |
Long-Lasting Healing: Can TMS Provide Lasting Relief?
For many people – yes. TMS therapy for PTSD and trauma produces improvements that tend to hold well past the treatment window, though it’s not a permanent fix for everyone. Research in Frontiers in Psychiatry found that rTMS gains were often sustained for up to three months post-treatment, with some patients holding on much longer. How durable the results are depends on trauma severity, whether complex PTSD is involved, and whether TMS is paired with ongoing therapy.
Maintenance sessions are an option for patients who notice symptoms returning – similar to how periodic therapy helps some people stay on track.
The Benefits of TMS Over Traditional PTSD Treatments
For people who’ve tried multiple medications and therapy without enough lasting change, TMS approaches the problem differently:
- No systemic side effects – magnetic pulses don’t travel through the body like drugs do, avoiding the hormonal and metabolic effects that often derail medication treatment
- No sedation or memory risk – unlike ECT, TMS requires no anesthesia and has no association with memory loss
- Works on the root cause – rather than chemically masking symptoms, TMS recalibrates the brain circuits driving them
Road to Recovery: Building a Support System
TMS is a real piece of the recovery puzzle – but it works best as part of something bigger, not on its own.
Combining TMS Therapy with Other Support Systems
TMS pairs well with trauma-focused therapy. The changes it produces in the brain can lower the anxiety baseline enough that working through trauma in therapy feels more manageable – something that’s genuinely hard for many people to do without that foundation. Many providers who offer TMS therapy for PTSD suggest pairing it with CPT or EMDR around the same period.The basics matter too – steady sleep, reduced alcohol use, peer support, and stable relationships all help consolidate the progress TMS makes possible. Recovery isn’t linear, but TMS can give people a real foothold to build from.
Is TMS the Right Next Step?
For trauma survivors who’ve tried conventional treatments without lasting relief, TMS therapy for PTSD is a well-supported option worth taking seriously. The research points consistently toward meaningful symptom reduction, durable results, and a side-effect profile most patients handle well. With the right support around it, TMS has real potential to shift things for people who’ve felt stuck for a long time.
If that sounds like you – or someone you care about – LifQuality TMS is a good place to start. Their team can help determine whether TMS treatment for PTSD fits your specific history and goals. Get in touch by emailing info@lifequalitytms.com or calling (718) 400-0867– sometimes one honest conversation opens a door that’s been closed for years.
Frequently Asked Questions
1. Is TMS covered by insurance for PTSD?
Coverage varies. Many plans cover TMS for depression, and PTSD coverage is expanding as the evidence grows. It’s worth calling your insurer directly to ask. Many providers also offer financing options.
2. How many TMS sessions are needed for PTSD?
Most courses involve 20 to 36 sessions over four to six weeks. Some protocols – particularly deep TMS for PTSD – use accelerated schedules with two sessions per day over a shorter timeframe.
3. Can TMS be used for complex PTSD?
Yes – TMS for complex PTSD is an active area of clinical interest. The same brain circuits are involved, and early results are encouraging, especially when TMS is combined with trauma-focused therapy.
4. Does TMS work if medications haven’t helped?
This is actually where TMS often performs best. Since it works through neural stimulation rather than chemistry, patients who haven’t responded to antidepressants are often strong candidates.
5. Are there side effects with TMS therapy?
TMS is generally well-tolerated. The most common complaints are mild scalp discomfort or headaches during the first week, which typically fade. Serious adverse events like seizures are rare, and – unlike ECT – there’s no memory loss risk.
