You’ve tried multiple antidepressants. Maybe Zoloft gave you crippling fatigue. Lexapro killed your sex drive. Wellbutrin triggered anxiety. Effexor worked for a while, then stopped. Now your psychiatrist is suggesting yet another medication, and you’re wondering: isn’t there a better way?
There is. The debate between TMS vs medication vs alternative depression treatments represents one of the most important conversations in modern depression treatment. While antidepressants remain a first-line option for many people, Transcranial Magnetic Stimulation offers a fundamentally different approach – one that targets depression at its source without introducing chemicals into your system.
This comprehensive guide explores how TMS treats depression without medication, examines the science behind combining medication with TMS therapy, and helps you understand why an increasing number of people are choosing TMS therapy over medications.
Understanding the Basics: How Each Treatment Works
Before comparing TMS vs medication (antidepressants) for depression, it’s essential to understand how each approach works in your brain.
How Antidepressant Medications Work
Antidepressants function by altering neurotransmitter levels throughout your entire brain and body. Different classes work through various mechanisms:
- SSRIs (Selective Serotonin Reuptake Inhibitors) like Prozac, Zoloft, and Lexapro increase serotonin availability by blocking its reabsorption
- SNRIs (Serotonin-Norepinephrine Reuptake Inhibitors) like Effexor and Cymbalta affect both serotonin and norepinephrine systems
- Atypical antidepressants like Wellbutrin work on dopamine and norepinephrine pathways
- Tricyclics and MAOIs, older medications typically reserved for treatment-resistant cases, affect multiple neurotransmitter systems
These medications work systemically, meaning they affect your entire body – not just the brain regions involved in depression. This systemic approach explains both their benefits and their numerous side effects.

How TMS Treats Depression Without Medication
TMS treatment without medication takes a completely different approach. Instead of flooding your system with chemicals, TMS uses targeted magnetic pulses to stimulate specific underactive brain regions associated with depression.
Here’s how TMS treats depression without medication:
- Precise targeting: A magnetic coil positioned against your scalp delivers pulses directly to the left dorsolateral prefrontal cortex – the brain region showing decreased activity in depression.
- Neural activation: These magnetic pulses generate small electrical currents that stimulate nerve cells, increasing their activity and connectivity.
- Natural chemistry: Rather than introducing external chemicals, TMS prompts your brain to naturally regulate its own neurotransmitter production and neural circuits.
- Localized effect: Unlike medications that affect your entire system, TMS targets only the specific brain areas involved in mood regulation.
According to research from Harvard Medical School, approximately 50-60% of people who haven’t responded to medication experience significant improvement with TMS, with about one-third achieving complete remission.
TMS vs Medication: A Comprehensive Side-by-Side Comparison
Let’s break down the key differences between TMS and medication across multiple factors that matter most to people seeking depression treatment.
| Factor | TMS Therapy | Antidepressant Medication |
| Effectiveness | 50-60% response rate in treatment-resistant depression; 30-40% achieve complete remission | 33-37% complete remission; highly variable depending on medication class and individual response |
| Side Effects | Mild scalp discomfort, temporary headache; no systemic effects, weight changes, or sexual dysfunction | Weight gain, sexual dysfunction, nausea, sleep issues, emotional blunting, digestive problems; 40-50% report troublesome side effects |
| Treatment Duration | 4-6 weeks of daily sessions; results often last 12+ months; maintenance sessions available if needed | Ongoing daily medication; typically 6+ months minimum; many require years of continuous use |
| Time to Results | Improvement typically begins within 2-3 weeks | Usually requires 4-8 weeks to assess effectiveness |
| Impact on Daily Life | 20-minute sessions; no recovery time; drive yourself; return to work immediately | Must remember daily pill; possible impact on energy, cognition, sexual function affects daily activities |
| Cost | Higher upfront cost; covered by most insurance for treatment-resistant depression; potentially lower lifetime costs | Lower monthly cost; ongoing expenses; cumulative costs increase with long-term use |
Why Choose TMS Therapy Over Medications
Given the data, why are more people choosing TMS therapy over medications? The answer lies in both the unique benefits TMS offers and the limitations many experience with antidepressants.
Freedom from Systemic Side Effects
Perhaps the most compelling reason to choose TMS therapy over medications is the dramatic difference in side effects. While 40-50% of people taking antidepressants report troublesome side effects, TMS side effects are minimal and localized.
Consider what you won’t experience with TMS:
- No weight gain: Antidepressants commonly cause 10-25 pound weight increases; TMS doesn’t affect metabolism or appetite
- No sexual dysfunction: Up to 70% of SSRI users experience decreased libido, difficulty achieving orgasm, or erectile problems; TMS has zero impact on sexual function
- No emotional blunting: Many describe feeling “flat” or numb on medications; TMS preserves your full emotional range
- No cognitive impairment: Medications can cause brain fog or memory issues; TMS actually improves cognitive function in many patients
- No digestive problems: Nausea, constipation, and diarrhea plague many on antidepressants; TMS doesn’t affect your GI system
- No sleep disruption: Medications can cause insomnia or excessive sleepiness; many TMS patients report improved sleep quality
The most common TMS side effect? Mild scalp discomfort during the first few sessions, which typically fades as treatment progresses. That’s it.
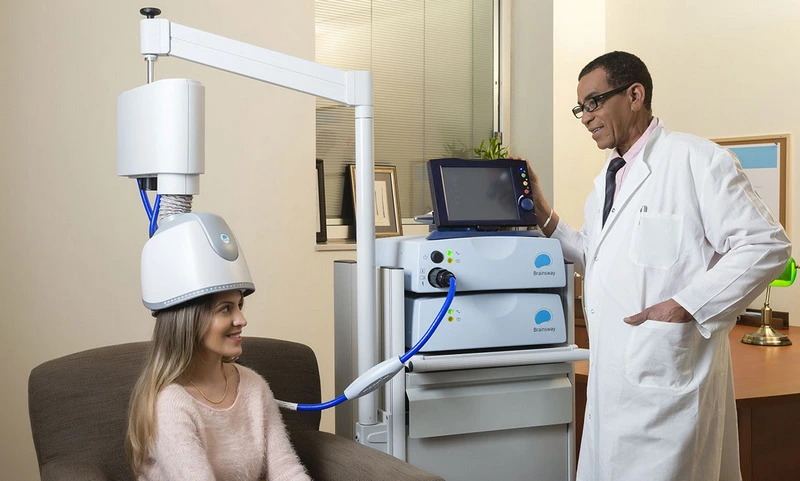
Targeted Treatment vs. Systemic Medication
When comparing TMS vs medication, one fundamental difference stands out: precision. Antidepressants work systemically, affecting serotonin receptors throughout your entire brain, gut, and body. TMS, by contrast, targets only the specific brain regions involved in depression.
This precision explains why TMS treatment without medication can be so effective while avoiding the widespread side effects of systemic drugs. You’re treating the problem at its source rather than flooding your system with chemicals that affect far more than just mood regulation.
Lasting Results Without Daily Maintenance
Unlike antidepressants that require daily adherence indefinitely, TMS offers lasting benefits after a defined treatment course. Research shows:
- Average duration of symptom relief extends beyond one year after TMS treatment ends
- Many patients maintain improvement for years without additional intervention
- If symptoms return, maintenance TMS sessions (much less frequent than the initial course) can restore benefits
- No withdrawal syndrome when treatment ends, unlike the difficult discontinuation process many face with antidepressants
This means freedom from the daily ritual of medication, the worry about running out of pills, and the challenge of maintaining perfect adherence.
Proven Effectiveness for Treatment-Resistant Depression
Perhaps the strongest reason why people choose TMS therapy over medications is simple: TMS works when medications have failed. Studies consistently show that 50-60% of people who haven’t responded to multiple antidepressants experience significant improvement with TMS.
Real-world data from Life Quality TMS and other centers often exceeds these numbers. Many clinics report response rates of 70-80% when using advanced deep TMS technology like BrainsWay, which reaches deeper brain structures than traditional TMS.
Combining Medication with TMS Therapy: The Best of Both Worlds
While many people seek TMS specifically to avoid medication, combining medication with TMS therapy can produce superior results for some patients. This isn’t an either-or decision – it’s about finding what works best for your unique situation.
The Science Behind Combining Medication with TMS Therapy
Groundbreaking research published in The Lancet’s eClinicalMedicine reveals that combining medication with TMS therapy – particularly SSRIs with TMS – produces significantly better outcomes than either treatment alone.
Key findings include:
- TMS combined with SSRIs showed large, significant improvements in depression scores compared to SSRI monotherapy
- Response rates and remission rates both increased substantially with combination therapy
- The synergistic effect suggests TMS and SSRIs work through complementary mechanisms
- A study found that deep TMS combined with antidepressants achieved higher remission rates than medication alone
Why does combining medication with TMS therapy work so well? The two approaches target depression through different mechanisms:
- Medications increase neurotransmitter availability throughout the brain
- TMS stimulates specific neural circuits and improves brain connectivity
- Together, they address both the chemical and circuit-level dysfunction in depression

Who Benefits Most from Combining Medication with TMS Therapy
Combination therapy particularly helps:
- People with severe depression who had partial but incomplete response to medication alone
- Those experiencing medication benefits but wanting to enhance results and possibly reduce dosage
- Individuals who’ve found a tolerable medication but need additional improvement
- Patients transitioning off medication who use TMS to maintain stability during tapering
At Life Quality TMS, we support patients whether they’re using TMS as a standalone treatment or combining medication with TMS therapy. Our psychiatrists work collaboratively with you and your existing providers to create the most effective treatment plan.
Using TMS to Taper Off Medications Safely
Many people start combining medication with TMS therapy with a long-term goal: eventually reducing or eliminating medication. TMS provides a bridge to medication-free mental health.
The typical process:
1. Begin TMS while maintaining current medication: This ensures you don’t lose ground while starting treatment.
2. Monitor improvement over 4-6 weeks: Most people notice significant benefits by this point.
3. Complete TMS course and stabilize: Allow 2-3 months after treatment ends to ensure benefits are sustained.
4. Work with your psychiatrist to gradually taper medication: Slow reduction minimizes withdrawal symptoms and monitors for any depression recurrence.
5. Use maintenance TMS if needed: Periodic booster sessions can maintain benefits long-term.
Important: Never discontinue antidepressants abruptly. Always work with your healthcare provider to create a safe tapering plan.
Making Your Decision: TMS vs Medication for Depression
So how do you decide between TMS vs medication for depression? Consider these factors:
You Might Be a Good Candidate for TMS If:
- You’ve tried at least two antidepressants without adequate improvement
- Medication side effects significantly impact your quality of life
- You prefer a drug-free approach or cannot take medications due to pregnancy, breastfeeding, or medical contraindications
- You’re concerned about long-term medication dependency
- You have treatment-resistant depression that hasn’t responded to standard approaches
- You want lasting results without daily medication maintenance
When Medication Might Be the Right First Step
Despite TMS’s advantages, medication remains appropriate for many people, especially:
- First episode of mild to moderate depression
- When immediate intervention is needed and TMS isn’t immediately accessible
- Cost or insurance coverage makes medication significantly more accessible
- You’ve previously responded well to medication with minimal side effects
- Time commitment for daily TMS sessions isn’t feasible in your current life situation
The key is working with knowledgeable providers who understand both options and can guide you toward the best approach for your unique circumstances.
Ready to Explore Your Options?
The decision between TMS vs medication doesn’t have to be complicated. It comes down to finding the treatment that works best for your body, your life, and your goals for mental health.
If you’re tired of medication side effects, frustrated by treatment-resistant depression, or simply want to explore how TMS treats depression without medication, we’re here to help.
Call (718) 400-0867 today to schedule your consultation. Let’s discuss whether TMS, medication, or a combination approach is right for you.
Frequently Asked Questions About TMS vs Medication
Is TMS better than antidepressants?
Neither treatment is universally “better”. Each has advantages depending on your situation. TMS offers superior side effect profile, lasting results after a defined treatment course, and effectiveness for treatment-resistant depression. Antidepressants provide easier accessibility, lower upfront cost, and proven effectiveness for many people. For treatment-resistant depression specifically, research shows TMS achieves 50-60% response rates even when medications have failed, making it exceptionally valuable for this population.
Can I do TMS while taking antidepressants?
Yes, absolutely. Combining medication with TMS therapy is not only safe but often produces better results than either treatment alone.
How long do TMS results last compared to medication?
TMS results typically last 12+ months on average, with many patients maintaining improvement for several years. If symptoms gradually return, maintenance TMS sessions can restore benefits. Medication requires continuous daily use – stopping medication often leads to symptom return within weeks to months.
How does deep TMS compare to regular TMS and medication?
Deep TMS (like the BrainsWay system used at Life Quality TMS) reaches deeper brain structures and covers more extensive areas than traditional TMS, potentially providing superior results. Real-world data shows response rates of 70-80% with deep TMS compared to 50-60% with traditional TMS. When compared to medication, deep TMS offers the same advantages as standard TMS (no systemic side effects, lasting results) with even stronger effectiveness data for treatment-resistant cases.
Can TMS help if I’ve been on antidepressants for years?
Yes, TMS frequently helps people who’ve been on antidepressants long-term, whether you still experience symptoms despite medication or you’ve become dependent on medication to maintain stability. Many patients use TMS to enhance medication benefits, then gradually taper under medical supervision. Long-term medication use doesn’t reduce TMS effectiveness – in fact, TMS may work particularly well for medication-experienced patients by addressing aspects of depression that pharmacotherapy doesn’t fully reach.