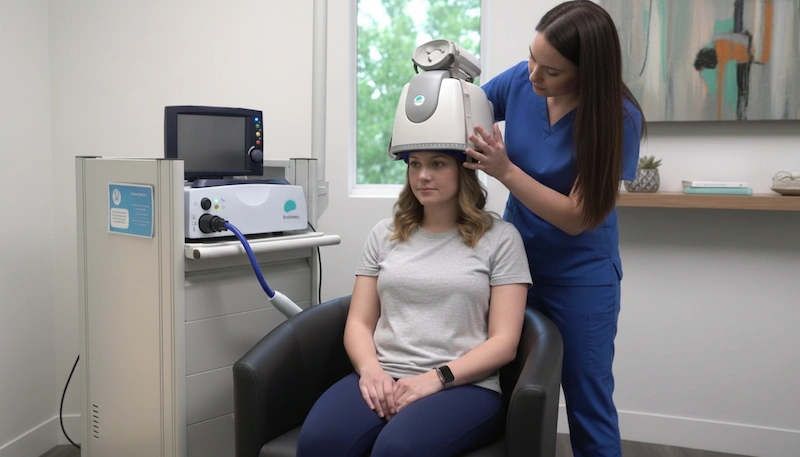
If you or someone you love has been struggling with depression, OCD, or anxiety, you may have come across transcranial magnetic stimulation (TMS) as a treatment option. But here’s something many people don’t realize at first: TMS is not a single, one-size-fits-all therapy.
The way TMS is delivered – the frequency, intensity, duration, and even the type of coil used – can vary significantly depending on the condition being treated and the individual’s needs. These delivery methods are called TMS protocols, and understanding them can help you make a more informed decision about your care.
What Are TMS Protocols and Why Do They Matter?
A TMS protocol is essentially the “prescription” for how a TMS treatment session is structured. It defines parameters like the frequency of magnetic pulses, the number of pulses per session, the length of each session, how many sessions are needed, and which area of the brain is targeted. Getting these parameters right is what makes TMS effective. The same technology, applied differently, can produce different outcomes for different patients and conditions.
TMS was first FDA-approved in 2008 for major depressive disorder (MDD). Since then, researchers and clinicians have developed and refined multiple protocols to expand what TMS can treat and improve how quickly and effectively it works. Today, there are several distinct approaches – each with its own clinical evidence base.
The Main Types of TMS Protocols
Standard Repetitive TMS (rTMS)
Standard repetitive TMS, or rTMS, is the original FDA-approved protocol and remains one of the most thoroughly studied approaches. It delivers magnetic pulses at a consistent frequency to the left dorsolateral prefrontal cortex (DLPFC), a brain region associated with mood regulation. Sessions typically last around 20 to 40 minutes and are administered five days a week for four to six weeks.
High-frequency rTMS (usually 10 Hz) over the left DLPFC is the most widely used and best-supported approach for depression. Research has consistently shown that high-frequency rTMS over the left DLPFC is superior in antidepressant effect when compared to other stimulation patterns. A lower-frequency variant (1 Hz) applied to the right DLPFC is also used, often for patients who tolerate high-frequency stimulation less well.
Theta Burst Stimulation (TBS)
Theta burst stimulation is a newer, faster variation of TMS. Instead of evenly spaced pulses, TBS delivers rapid bursts of high-frequency stimulation in patterns that mimic naturally occurring brain rhythms. TBS reduces session duration while maintaining therapeutic efficacy, offering a more time-conscious option for patients without compromising treatment outcomes.
There are two main forms. Intermittent theta burst (iTBS) is excitatory – it activates target neurons – and is commonly used for depression. Continuous theta burst (cTBS) is inhibitory, meaning it tends to reduce activity in the targeted area, and is used in other clinical applications. iTBS sessions can take just over 3 minutes while maintaining efficacy comparable to standard 37-minute protocols, which may also improve treatment adherence.
Accelerated TMS Protocol
The accelerated TMS protocol condenses treatment into a much shorter timeframe by delivering multiple TMS sessions per day, rather than one. Accelerated TMS is defined as a protocol delivering more than one daily TMS session, aimed at reducing treatment duration and improving response time, with the goal of achieving similar or superior levels of efficacy.
Accelerated TMS is particularly appealing for those who need fast symptom relief, including students, professionals, or those traveling from out of town. It also shows promise for treatment-resistant cases where a more intensive approach may be beneficial. This format is particularly relevant for individuals who cannot commit to a six-to-nine-week daily schedule.
Deep TMS (dTMS)
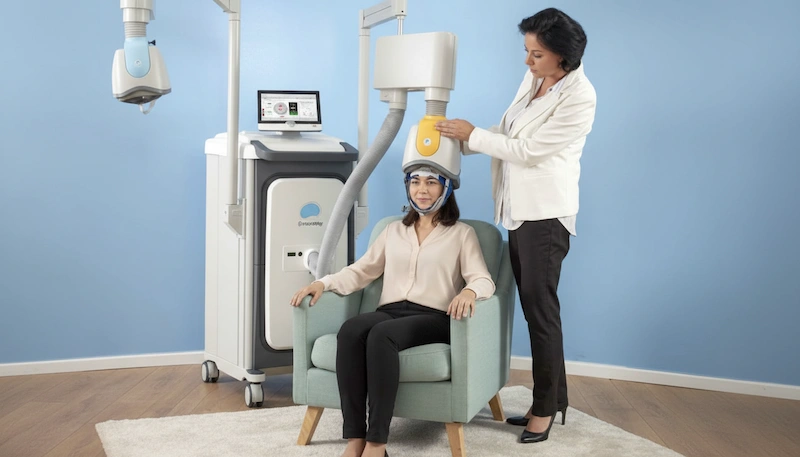
Deep TMS uses a specialized coil design – most notably the H-coil developed by BrainsWay – that allows magnetic pulses to reach deeper and wider areas of the brain than conventional surface coils. While standard rTMS is limited to cortical tissue, deep TMS reaches subcortical neurons, expanding its potential therapeutic scope.
Deep TMS was FDA-approved in 2013, and its session time is approximately half that of standard rTMS. At LifeQuality TMS in Brooklyn, we use the BrainsWay Deep TMS system – the same technology that has been validated in multiple FDA-cleared clinical trials for depression, OCD, and smoking cessation.
Comparing TMS Protocols at a Glance
| Protocol | Session Length | Treatment Duration | FDA-Approved For |
| Standard rTMS | 20-40 min | 6-9 weeks | Depression (MDD) |
| Theta Burst (iTBS) | 3-10 min | 6-9 weeks | Depression (MDD) |
| Accelerated TMS | 3-10 min/session, multiple/day | 1-2 weeks | Depression (MDD) |
| Deep TMS (dTMS) | ~20 min | 4-6 weeks | Depression, OCD, Smoking Cessation |
Condition-Specific TMS Protocols
OCD TMS Protocol: Targeting Deeper Neural Circuits
The OCD TMS protocol is meaningfully different from depression protocols. OCD is linked to overactivity in specific circuits connecting the prefrontal cortex to deeper brain structures – and reaching those areas requires a different approach. Conventional TMS coils cannot directly target the cortico-striato-thalamo-cortical circuits associated with OCD, but deep TMS apparently can.
BrainsWay’s Deep TMS using the H7-coil is the first and, for a long time, only non-invasive device to receive FDA clearance for OCD treatment. A peer-reviewed multicenter clinical study found that after 29 sessions, nearly 60% of patients achieved a response (defined as more than 30% reduction in OCD symptom severity), and over 70% of patients reached their first response after an average of 18.5 sessions.
One distinctive feature of the OCD TMS protocol is symptom provocation: before each session, patients are briefly exposed to their anxiety triggers to activate the relevant brain circuits, making stimulation more targeted and effective. BrainsWay Deep TMS treatment has been shown to be safe and effective in the treatment of patients with OCD, with improvement typically occurring by the second week of treatment for those who benefit.
ADHD TMS Protocol: An Emerging Area of Research
The ADHD TMS protocol is a developing field, with growing evidence that TMS can help regulate the prefrontal circuits involved in attention and impulse control. ADHD involves dysfunction in the frontal and prefrontal regions of the brain – the same areas TMS is well-positioned to target.
While TMS for ADHD is not yet FDA-approved as a standalone treatment, clinical research is actively expanding. Deep TMS has shown promise for adult ADHD, with research suggesting that targeting specific brain regions can produce meaningful improvements in attention and executive function. Patients interested in the ADHD TMS protocol should discuss current research and eligibility with their provider.
TMS Treatment Protocol for Depression: Tailored to Severity
For depression, the TMS treatment protocol is selected based on the severity of symptoms, previous treatment history, and patient schedule. Standard rTMS and deep TMS are both well-established. For patients who have responded to an acute TMS treatment course, maintenance protocols – involving periodic sessions after initial treatment – have also shown significant efficacy in decreasing the risk of relapse.
At LifeQuality TMS, our clinical team evaluates each patient individually to determine the most appropriate approach, whether that means a standard protocol, deep TMS, or a maintenance plan for long-term symptom management.

Customized TMS Protocols
Custom TMS protocols refer to treatment plans adjusted beyond standard parameters to fit a specific patient’s brain physiology, diagnosis, or response to treatment. These adjustments can include changes to stimulation frequency, pulse intensity (calibrated to the patient’s motor threshold), session length, number of sessions, or the brain region targeted.
Personalization matters because no two brains – and no two cases of depression or OCD – are identical. Factors that may prompt customization include:
- Previous treatment-resistance to standard protocols
- Co-occurring diagnoses (for example, depression alongside OCD)
- Individual tolerance to stimulation intensity
- Response patterns observed during an initial treatment course
- The need for an accelerated schedule due to work or travel constraints
A well-designed customized TMS protocol balances clinical evidence with individual patient data, reviewed and adjusted by a qualified TMS physician throughout the course of treatment.
Key Factors That Define Any TMS Protocol
Whatever the protocol, all TMS treatment plans are built around the same core parameters. Understanding these gives patients a clearer picture of what their treatment involves:
- Stimulation frequency: High-frequency (≥5 Hz) is generally excitatory; low-frequency (1 Hz) is inhibitory. The choice depends on which brain region is targeted and the desired therapeutic effect.
- Motor threshold: The intensity of pulses is calibrated as a percentage of each patient’s motor threshold – the minimum stimulation needed to produce a visible finger twitch. Most TMS protocols stimulate at 120% of resting motor threshold, though some newer protocols adjust this individually using neuroimaging data.
- Number of pulses per session: Typically ranges from 600 to 3,000 pulses per session depending on the protocol.
- Total number of sessions: Standard courses range from 20 to 36 sessions; extended or maintenance protocols may add sessions beyond the initial course.
- Brain target: Left DLPFC for depression; medial prefrontal cortex and anterior cingulate cortex for OCD; other targets are under investigation for ADHD and anxiety.
How Providers Choose the Right TMS Protocol?
The selection of the right protocol is a clinical decision, made by a TMS physician after a full psychiatric evaluation. It involves reviewing the patient’s diagnosis, symptom severity, treatment history, and any contraindications. A TMS physician is required to have an extensive background in brain physiology and a deep understanding of the neurophysiological effects of rTMS, and the prescription of TMS is considered a specialized clinical skill.
At LifeQuality TMS, our licensed psychiatrists conduct a thorough evaluation before recommending any protocol. We also handle all insurance authorizations on behalf of our patients – because navigating coverage should not be an obstacle to getting the right care.
If you are in Brooklyn or the wider New York City area and want to explore whether TMS is right for you, contact our team to schedule a consultation.
Frequently Asked Questions About TMS Protocols
1. What is the most commonly used TMS protocol for depression?
The most widely used and well-researched protocol for depression is high-frequency repetitive TMS (10 Hz) delivered to the left dorsolateral prefrontal cortex. Deep TMS using the BrainsWay H1-coil is also FDA-approved for depression and reaches deeper brain structures than standard rTMS, which may benefit patients who have not responded to surface-level protocols.
2. How long does a typical TMS treatment protocol last?
Most standard TMS treatment protocols last between four and nine weeks, with daily sessions five days per week. The accelerated TMS protocol condenses this to as little as one to two weeks through multiple daily sessions. Your provider will recommend a duration based on your diagnosis, symptom severity, and response to treatment.
3. Can a TMS protocol be adjusted mid-treatment?
Yes. TMS protocols can be modified by the treating physician if a patient is not responding as expected, experiencing discomfort, or showing signs that a different approach may be more effective. This is one reason it is important to work with an experienced TMS provider who monitors progress throughout the course of treatment.
4. Are there TMS protocols for conditions other than depression and OCD?
Yes. TMS protocols have been studied for anxiety, PTSD, bipolar depression, ADHD, smoking cessation (FDA-cleared for BrainsWay), and other conditions. Not all of these have received FDA clearance, meaning some are used “off-label” based on available research. Always discuss the evidence base for any off-label protocol with your provider.
5. Does the type of TMS device affect which protocols are available?
Yes, significantly. Different devices use different coil types, which determines how deep and how broadly the magnetic field penetrates the brain. BrainsWay Deep TMS, which LifeQuality TMS uses, is unique in that its H-coil design enables both deeper and wider stimulation compared to the standard figure-eight coil. This is why it holds FDA clearance for a broader range of indications.