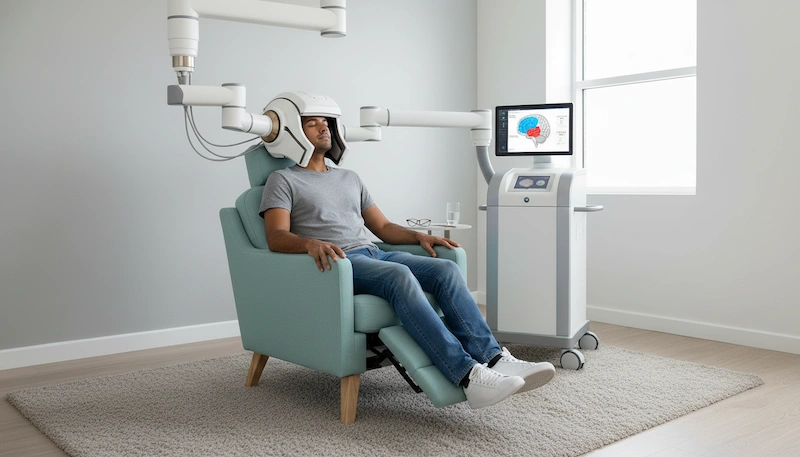
For people living with treatment-resistant depression, hearing that 80% of clinical trial participants went into remission after just five days of treatment sounds almost too good to be true. That is the claim behind SAINT TMS – a protocol that has generated significant excitement in the mental health field. But what exactly is it, how does it work, and is it right for you? This article breaks it down honestly, including what the evidence does and does not yet confirm.
What Is SAINT TMS?
SAINT TMS is an advanced, accelerated form of transcranial magnetic stimulation developed by researchers at Stanford University. The acronym stands for Stanford Accelerated Intelligent Neuromodulation Therapy. It was developed by Dr. Nolan Williams and his team at the Stanford Brain Stimulation Lab as a way to dramatically shorten treatment time and improve outcomes for patients with major depressive disorder (MDD) – especially those who have not responded to antidepressant medications.
The SAINT protocol TMS approach differs from conventional TMS in two significant ways: first, it uses functional MRI (fMRI) to individually map each patient’s brain before treatment begins; and second, it delivers stimulation in an accelerated, intensive format – multiple short sessions per day over just five consecutive days.
Traditional TMS protocols for depression typically involve one session per day, five days a week, for six to nine weeks. SAINT compresses what would otherwise be a multi-week commitment into a single working week.
How Does the SAINT Protocol Work?
Step 1: Brain Mapping with fMRI
Before any stimulation begins, patients undergo an fMRI scan to identify the precise location of their dorsolateral prefrontal cortex (DLPFC), the brain region most associated with mood regulation and depression. This matters because the exact location of the DLPFC varies from person to person by as much as several millimeters. Without imaging-guided targeting, this area is sometimes missed when standard positioning methods are used, which can reduce treatment effectiveness. The fMRI data is then used with neuronavigation equipment to guide the placement of the TMS coil during each session.
Step 2: Accelerated Stimulation Over Five Days
The SAINT TMS treatment itself consists of 10 stimulation sessions per day over five consecutive days – 50 sessions in total. Each session uses intermittent theta burst stimulation (iTBS), a rapid pattern of magnetic pulses that takes under 10 minutes to deliver. Sessions are spaced approximately 50 minutes apart throughout the day.
This gives the brain repeated, closely timed stimulation – an approach informed by neuroscience research showing that intervals of this length may be optimal for producing long-term changes in neural connectivity. Each patient also receives 1,800 pulses per session, which is three times the number used in the standard once-daily iTBS protocol that received earlier FDA clearance.
Why the Combination Matters
The combination of personalized targeting and high-dose accelerated delivery is what distinguishes the Stanford TMS protocol from both conventional rTMS and standard iTBS. Precision ensures the right brain region is stimulated; intensity and repetition are designed to produce deeper and faster neuroplastic changes. According to Stanford Health Care, SAINT can improve depression symptoms significantly faster than other types of TMS therapy.
What Does the Clinical Evidence Show?
Clinical Trial Results
The SAINT TMS protocol has been evaluated in several clinical studies. In an early open-label pilot study, 90% of participants with treatment-resistant depression met remission criteria immediately after completing the five-day course. A subsequent double-blind, randomized controlled trial published in the American Journal of Psychiatry found that 79% of participants achieved remission at some point in the four weeks following treatment, compared to only 13.3% in the sham group.
These are notably high numbers, especially given that all participants had already failed to respond to at least one antidepressant medication. The improvements were also described as rapid – patients and researchers observed meaningful changes in mood within days of beginning treatment.
Important Caveats
Those results are genuinely exciting. But they come with important context. The original trials were conducted at Stanford with carefully selected patients and highly controlled conditions. Researchers have acknowledged that these results require replication across larger and more diverse populations before broader conclusions can be drawn.
Some studies conducted at independent sites outside of Stanford have reported lower remission rates, suggesting that results may vary depending on the clinical setting, patient selection criteria, and the precision of the fMRI-guided targeting process. The field is still in the process of standardizing the protocol for wider clinical use.
FDA Clearance: What It Means – and What It Doesn’t
SAINT received FDA clearance in September 2022 through a 510(k) pathway, granted to Magnus Medical (the company commercializing the Stanford-developed protocol) as a breakthrough device for adults with MDD who have not adequately responded to antidepressant medications. This is an important distinction to understand.
FDA clearance is not the same as full FDA approval, which is generally required before commercial insurance agrees to pay for a modality of treatment. Full approval typically requires a longer track record of post-market safety and efficacy data. As a result, insurance coverage for SAINT TMS treatment has remained very limited. Most insurance plans do not yet offer coverage for this type of treatment, meaning it is currently a self-pay option for most patients, often ranging from $6,000 to $10,000 for a full course – though this is changing gradually.
In 2025, the Centers for Medicare and Medicaid Services established specific hospital outpatient payment codes for SAINT treatment, signaling that payers are beginning to build reimbursement pathways for this approach. A small number of private insurers have also begun approving prior authorizations in certain settings, but coverage remains variable and is not yet widespread.
Who May Be a Candidate for SAINT TMS?
SAINT was designed specifically for adults with major depressive disorder who have not responded adequately to antidepressant medications. It may be particularly relevant for patients who:
- Have tried multiple antidepressants without sufficient relief
- Cannot commit to six to nine weeks of daily TMS sessions due to scheduling constraints
- Need rapid symptom improvement – for example, patients in inpatient or acute care settings
- Are willing and able to pay out of pocket, given current insurance limitations
- Do not have contraindications to MRI scanning (required for brain mapping)
SAINT is not currently FDA-cleared for conditions other than MDD, and it is not widely available outside of specialized centers.
How SAINT TMS Compares to Other TMS Approaches
| Feature | Standard rTMS | SAINT TMS Protocol | Deep TMS (BrainsWay) |
| Session length | 20-40 min | ~10 min per session | ~20 min |
| Sessions per day | 1 | 10 | 1 |
| Total treatment duration | 6-9 weeks | 5 days | 4-6 weeks |
| Brain targeting | Anatomical landmarks | fMRI-guided, individualized | H-coil, wider/deeper field |
| FDA status | Cleared (2008) | Cleared (2022, breakthrough) | Cleared (2013+) |
| Insurance coverage | Widely covered | Very limited, variable | Widely covered |
| Conditions treated | Depression | Depression (MDD) | Depression, OCD, Smoking |
SAINT TMS: Key Takeaways
SAINT TMS is a genuinely promising development in depression care – one worth understanding, especially for patients with treatment-resistant MDD. Its accelerated format and precision targeting set it apart from conventional TMS protocols. However, limited availability, inconsistent insurance coverage, and a still-growing evidence base mean it is not yet a practical option for most people seeking help today.
If you are exploring TMS for depression or other mental health conditions and want to understand which protocol may be right for you, the team at LifeQuality TMS in Downtown Brooklyn is here to help. We offer BrainsWay Deep TMS – FDA-cleared for depression, OCD, and smoking cessation, and accepted by most major insurance plans. Schedule a consultation today.
Frequently Asked Questions About SAINT TMS
1. Is SAINT TMS FDA approved?
SAINT received FDA clearance in September 2022 as a breakthrough device for treatment-resistant major depressive disorder. This is different from full FDA approval. Clearance means the device is legally permitted for clinical use, but it does not carry the same level of post-market evidence review as a full approval. Insurance coverage remains limited as a result.
2. How is the Stanford TMS protocol different from regular TMS?
The SAINT protocol TMS approach differs in two key ways: it uses fMRI brain imaging to individually target stimulation, and it delivers 10 sessions per day over five days rather than one session per day over several weeks. This makes it both more precise and significantly faster than standard TMS protocols.
3. What are the reported remission rates for SAINT TMS treatment?
In the double-blind controlled trial that supported FDA clearance, approximately 79% of participants in the active treatment group achieved remission at some point during the four weeks following treatment. However, independent replications have reported more modest outcomes, and results are expected to vary by clinical setting and patient characteristics.
4. Are there alternatives to SAINT for treatment-resistant depression?
Yes. Deep TMS, such as the BrainsWay system, is an FDA-cleared alternative for depression that reaches deeper brain structures than standard TMS and has a well-established clinical evidence base. It is more widely available and covered by most major insurers.
5. Can SAINT TMS treat OCD or anxiety?
At this time, SAINT TMS is only FDA-cleared for major depressive disorder. Other TMS protocols – including deep TMS with the BrainsWay H7-coil – have separate FDA clearances for conditions such as OCD. Patients seeking TMS for conditions beyond depression should discuss available options with their provider.