Generalized Anxiety Disorder (GAD) is not simply worrying too much. It is a clinical condition defined by persistent, excessive worry that feels difficult or impossible to control—often about multiple areas of life at once, including health, finances, relationships, and everyday responsibilities.
GAD accounts for an enormous share of the global mental health burden. What makes it particularly challenging is that many people with GAD normalize their symptoms for years before seeking help. When treatment is pursued, the path forward isn’t always obvious. This article outlines what the current evidence says about which treatments for generalized anxiety disorder to prioritize—and in what order.
First-Line Treatments for Generalized Anxiety Disorder (Start Here)
Cognitive Behavioral Therapy (CBT) as the Core Approach
CBT is widely regarded as the gold-standard psychological treatment for GAD, and the evidence supporting that designation is substantial. A large network meta-analysis published in JAMA Psychiatry concluded that CBT represents the first-line therapy for GAD based on both acute and long-term effectiveness across all reviewed psychotherapies.
The durability of those gains is one of CBT’s most clinically meaningful features. A 2025 follow-up study of two randomized controlled trials found that between 57% and 77% of patients were categorized as recovered two to eight years after completing CBT for GAD—a striking long-term outcome for a condition that tends toward chronicity.
CBT for GAD typically targets the following patterns:
- Cognitive restructuring — identifying and challenging catastrophic or distorted thinking about perceived threats
- Worry exposure — deliberately confronting feared scenarios to reduce avoidance and habituate the anxiety response
- Behavioral activation — rebuilding engagement with meaningful activities that worry and avoidance have progressively eliminated
- Intolerance of uncertainty — working through the core belief that uncertainty itself is dangerous or unacceptable
Individual face-to-face CBT consistently outperforms group and remote formats, though all structured formats produce better outcomes than no treatment. For those who need a specialized anxiety treatment approach, combining CBT with brain-based interventions can amplify results significantly.
Interventions That Actually Make a Difference
Lifestyle changes are rarely discussed with the seriousness they deserve in the context of GAD treatment. The evidence for several specific interventions is stronger than most people assume.
- Regular aerobic exercise is among the most consistently supported non-pharmacological interventions for anxiety. It modulates the HPA axis, reduces cortisol reactivity, and increases levels of brain-derived neurotrophic factor—biological shifts that directly reduce anxiety symptoms. The effect is not subtle. Even short bouts of moderate exercise produce measurable reductions in acute anxiety.
- Sleep hygiene is equally underestimated. GAD and sleep disruption share a particularly destructive relationship: anxiety fuels insomnia, and poor sleep worsens anxiety sensitivity the following day. Structured sleep interventions—consistent wake times, limiting caffeine after midday, reducing screen exposure before bed—address the physiological substrate of anxiety rather than just its surface symptoms.
- Caffeine reduction is a third lifestyle lever with direct clinical relevance. Caffeine is an adenosine antagonist that increases cortical arousal and can directly amplify the physiological features of anxiety, including heart rate elevation and heightened vigilance. Many individuals with GAD consume caffeine without recognizing its contribution to their symptom severity.
Combining Therapy and Lifestyle for Better Results
Neither CBT nor lifestyle changes alone produces consistent remission in moderate-to-severe GAD. The combination, however, is meaningfully more powerful than either approach in isolation. When exercise becomes regular, sleep improves, and arousal levels decrease, the cognitive work of CBT becomes easier—individuals can engage with challenging material from a more regulated neurological state.
The practical implication: don’t wait until therapy feels “settled” to address lifestyle. Start both simultaneously.

General Anxiety Disorder Treatment Without Medication
Who Can Benefit from Non-Medication Approaches
Non-medication treatment for GAD is most appropriate for individuals with mild-to-moderate symptom severity, those who prefer to avoid pharmacotherapy, pregnant or breastfeeding individuals for whom medication risk is a concern, and people who have experienced intolerable side effects from anxiolytics or antidepressants.
It is also a legitimate first step for those newly diagnosed who want to understand whether structured intervention alone can manage their symptoms before adding medication.
Proven Non-Medication Treatments
The strongest evidence-based non-medication options for GAD include:
- Individual CBT — first-line recommendation across major clinical guidelines; robust evidence for both acute symptom reduction and long-term recovery
- Acceptance and Commitment Therapy (ACT) — a third-wave CBT variant that focuses on psychological flexibility and values-based action rather than symptom elimination; well-supported for GAD
- Applied relaxation — structured progressive muscle relaxation and controlled breathing techniques; evidence supports equivalence with cognitive approaches in some studies
- Mindfulness-Based Cognitive Therapy (MBCT) — particularly useful for individuals with recurrent anxiety episodes; builds metacognitive awareness and reduces reactivity to anxious thoughts
- Neurofeedback — trains self-regulation of brainwave patterns associated with anxiety; emerging evidence suggests it works best as a complement to primary treatment
Limitations of Non-Medication Treatment
Non-medication general anxiety disorder treatment without medication has real boundaries. For individuals with severe GAD, significant functional impairment, or co-occurring depression, medication often plays a necessary role in reducing symptom intensity enough to make psychological therapy feasible.
TMS Therapy for Anxiety: A Non-Medication Advanced Option
What Is TMS Therapy and How Does It Work?
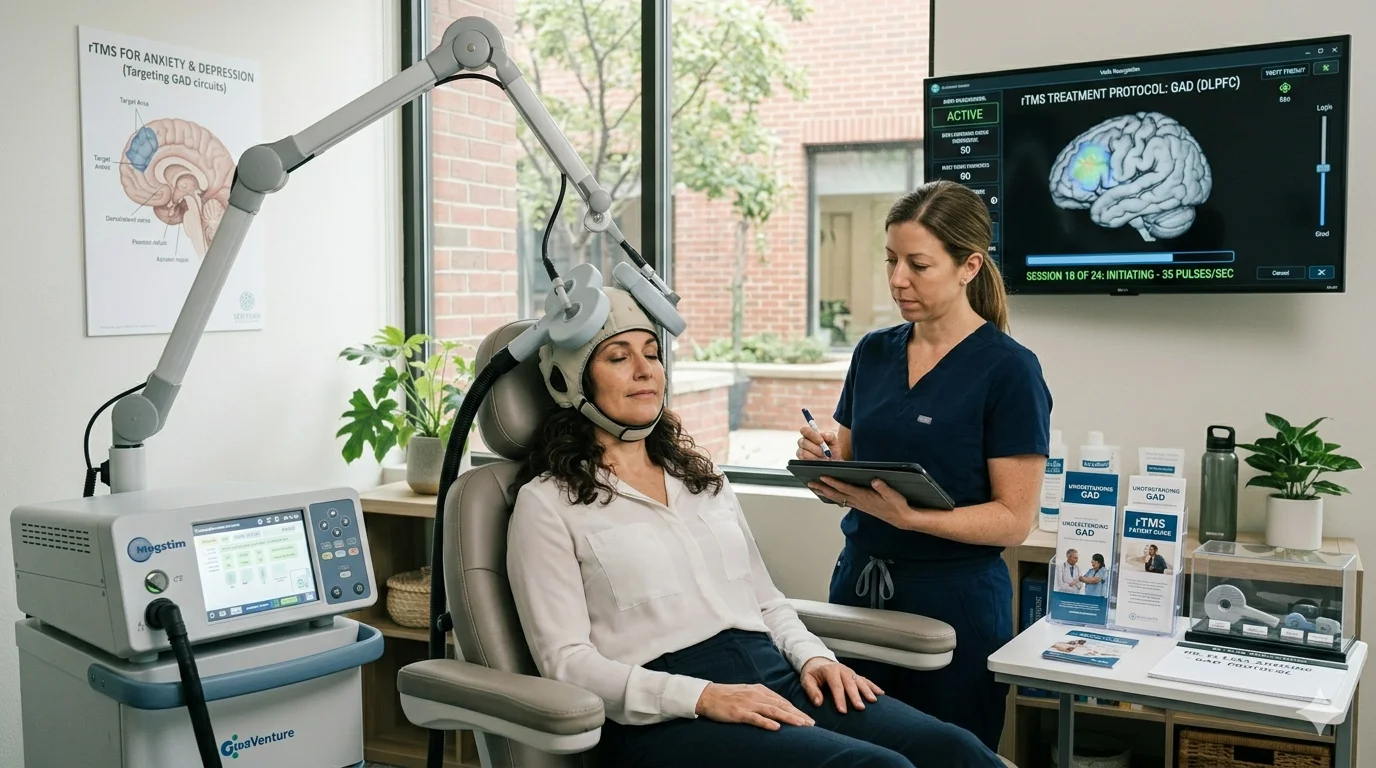
Transcranial Magnetic Stimulation (TMS) uses focused magnetic pulses to stimulate specific cortical regions involved in emotional regulation and anxiety modulation—primarily the dorsolateral prefrontal cortex (DLPFC). In GAD, research points particularly to right-hemisphere DLPFC stimulation as a target for reducing hyperarousal and the excessive cognitive load that characterizes persistent worry.
TMS is non-invasive, requires no sedation, and is administered in outpatient sessions typically lasting 20–40 minutes. A standard treatment course runs over several weeks. It does not carry the systemic side effects associated with medication, and no serious adverse events have been reported in clinical trials for anxiety. Learn more about what TMS treatment involves before booking a consultation.
When to Consider TMS in a Treatment Plan
TMS is particularly relevant for the following situations within a general anxiety disorder treatment plan:
- Partial response to CBT or medication — symptoms improved, but meaningful impairment persists
- Medication intolerance — GAD often co-occurs with depression, and many individuals cannot tolerate standard pharmacotherapy for either condition
- Treatment-resistant GAD — where multiple first-line options have been tried without adequate relief
- A preference for drug-free neurological intervention alongside ongoing therapy
TMS for GAD is also highly relevant when anxiety co-occurs with depression. Since LifeQuality TMS treats both depression and anxiety through targeted brain stimulation, individuals with co-occurring conditions may address both simultaneously within the same treatment course.
Benefits of TMS for Generalized Anxiety Disorder
The research on TMS for GAD has produced consistent and encouraging results. A systematic review and meta-analysis published in the International Journal of Neuropsychopharmacology found that rTMS decreased anxiety scores by an average of 1.857 standard deviations compared with sham treatment across included studies—a large effect size. The prediction interval did not include zero, indicating consistent anxiety-reducing effects across all comparable populations.
A separate large-scale meta-analysis of 208 randomized controlled trials, published in Molecular Psychiatry, confirmed significant positive effects of TMS for GAD symptoms (SMD = −1.8), with low heterogeneity—meaning the results were consistent rather than driven by outlier studies.
The key advantages of TMS for GAD:
- Drug-free mechanism — no systemic pharmacological exposure
- Targets the neurological source of anxiety dysregulation directly
- Can be combined with ongoing CBT or medication
- Well-tolerated with a favorable safety profile across clinical trials
Building a Personalized General Anxiety Disorder Treatment Plan
Matching Treatment to Severity
A well-structured treatment plan starts with an honest assessment of symptom severity. Mild GAD may respond well to structured CBT, exercise, and sleep intervention alone. Moderate GAD typically benefits from individual CBT as the primary intervention, with lifestyle changes as active support. Severe or treatment-resistant GAD warrants adding pharmacotherapy, TMS, or both—alongside ongoing psychological treatment.
The key principle: don’t undertreat. GAD that isn’t adequately addressed tends to become entrenched, and long-term chronicity makes recovery harder.
How to Adjust Based on Progress
Treatment response should be evaluated formally at regular intervals—typically every 4 to 8 weeks using standardized measures such as the GAD-7. If the response is insufficient at 8–12 weeks of consistent CBT, the next step is usually either medication augmentation or a brain-based intervention like TMS rather than simply continuing the same approach. Stagnation is information. A good treatment plan treats it as a signal to adapt.
Common Mistakes in Treatment Planning
Avoiding these mistakes significantly improves outcomes:
- Starting and stopping treatment inconsistently — GAD requires sustained engagement; sporadic participation undermines any intervention
- Treating anxiety in isolation — co-occurring depression, sleep disorders, or substance use need to be addressed concurrently, not sequentially
- Relying on medication alone — pharmacotherapy reduces symptoms but does not build the coping skills that prevent relapse; therapy is nearly always warranted alongside or instead of medication
- Dismissing advanced options too early — TMS and other brain-based approaches are not last resorts; for some individuals, they belong earlier in the plan

FAQ: Treatments for Generalized Anxiety Disorder
What is the most effective treatment for generalized anxiety disorder?
Individual CBT has the strongest evidence base for GAD, with demonstrated effectiveness at both acute and long-term follow-up. For individuals who don’t respond adequately to CBT alone, TMS and medication can meaningfully augment outcomes.
Can GAD be treated without medication?
Yes, particularly for mild-to-moderate cases. CBT, lifestyle interventions, and brain-based treatments like TMS are all evidence-supported non-medication options. Severe GAD may require medication as part of the plan, at least initially.
How long does treatment for GAD take?
A standard course of individual CBT runs 12–16 sessions over three to four months. Lifestyle changes produce effects on a rolling basis as they are sustained. TMS is delivered over several weeks of outpatient sessions. Most people require some form of ongoing maintenance to prevent relapse.
What happens if first-line treatments don’t work?
Partial or non-response to CBT or medication is the trigger for escalating care—not a sign that recovery isn’t possible. TMS is a well-supported next step for treatment-resistant or partially responding GAD, and combining approaches often produces gains that neither achieves alone.
Is TMS covered by insurance for anxiety?
TMS is FDA-approved for depression and OCD. Coverage for anxiety varies by insurer and clinical presentation. A consultation with a TMS provider can clarify what documentation supports coverage in a given case.
Starting the Right Treatment at the Right Time
GAD responds best to consistent, guided care—not to waiting for symptoms to resolve on their own or cycling through treatments without a structured plan. If you’re exploring whether TMS therapy might fit into your treatment approach, contact LifeQuality TMS in Brooklyn to speak with a specialist about your options.