Depression, anxiety, and related mood disorders remain among the most treatment-resistant conditions in psychiatry. Medication helps many people — but not everyone. Roughly one in three people with major depressive disorder does not achieve adequate relief from antidepressants, even after multiple trials. Therapy narrows that gap further, yet a meaningful share of patients still experience persistent symptoms that substantially impair daily functioning, relationships, and quality of life.
This is where brain stimulation therapy enters the picture. Rather than altering neurochemistry through pharmacology, these approaches work directly on the neural circuits that drive mood, attention, and emotional regulation. They vary widely in mechanism, invasiveness, evidence base, and practical accessibility, which makes understanding the differences genuinely important before choosing a path.
How Brain Stimulation Affects the Brain
The core principle across all forms of brain stimulation therapy is circuit modulation. Mental health conditions like depression are increasingly understood not simply as chemical imbalances but as disruptions in specific neural networks — particularly the prefrontal-limbic circuits that regulate emotional processing, motivation, and executive function.
Brain stimulation approaches target these circuits directly, either by inducing electrical activity, delivering magnetic pulses, or modulating nerve pathways that connect to the brain’s mood-regulating regions.
Types of Brain Stimulation Therapy
Transcranial Magnetic Stimulation (TMS)
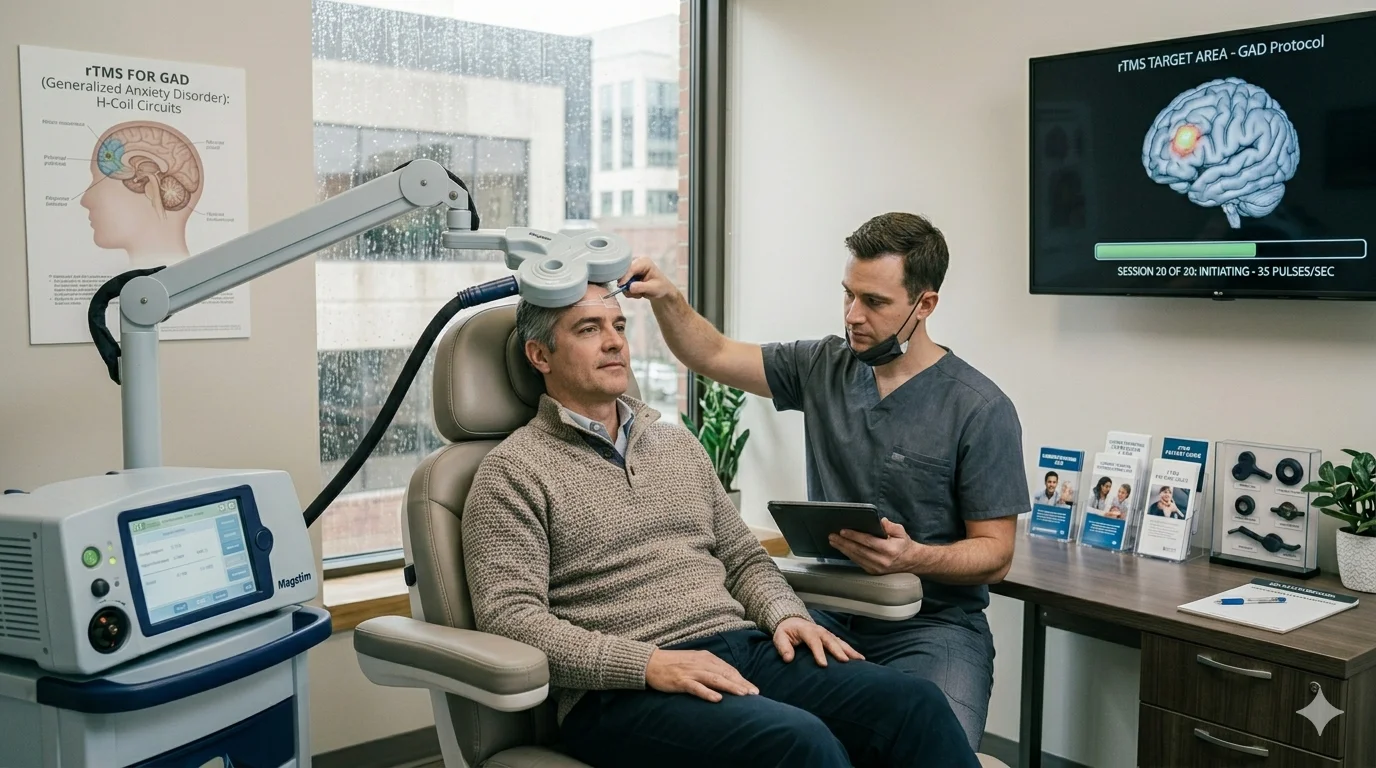
TMS uses a magnetic coil placed against the scalp to deliver focused magnetic pulses to the dorsolateral prefrontal cortex (DLPFC) — a region consistently underactive in depression and anxiety. The pulses are painless for most patients, require no anesthesia or sedation, and are administered in outpatient sessions lasting 20–40 minutes. A standard course runs over several weeks of daily sessions.
A 2025 consensus review endorsed by the National Network of Depression Centers, drawing on nearly 2,400 studies, confirmed that TMS is safe and effective even for individuals whose depression has not responded to medications, with up to 83% of patients showing measurable improvement in real-world settings. TMS is FDA-approved for major depressive disorder, OCD, and as of 2024, for adolescents aged 15 and up.
LifeQuality TMS in Brooklyn uses the BrainsWay deep TMS device, which reaches deeper cortical structures than traditional surface coils. Learn what TMS treatment involves before your first consultation.
Electroconvulsive Therapy (ECT)
ECT is the oldest and most effective brain stimulation therapy available for severe depression. It delivers a brief controlled electrical current through the scalp under general anesthesia, inducing a therapeutic seizure. Each session takes approximately one hour (including preparation and recovery), and treatment is typically administered two to three times per week for six to twelve sessions.
The significant limitation is its side effect profile. Memory disruption — both retrograde and anterograde — is the most commonly reported concern, and while it is typically temporary, it is clinically meaningful for many patients. ECT also requires anesthesia, hospital or clinical monitoring, and a recovery period after each session.
Vagus Nerve Stimulation (VNS)
VNS involves surgically implanting a small device under the skin of the chest that delivers electrical pulses to the vagus nerve, which carries signals from the body to the brain’s mood-regulating regions. The FDA approved an implanted VNS device for treatment-resistant depression in 2005, and a non-invasive transcutaneous version has since been developed.
VNS is typically reserved for patients with chronic, treatment-resistant depression who have not responded to multiple other interventions. Response tends to be slow — improvements often emerge over months rather than weeks — and the surgical implantation carries standard procedural risks. It is not a first-escalation option, but for appropriately selected patients, it can produce durable relief.
Deep Brain Stimulation (DBS)
DBS is the most invasive neuromodulation approach currently available. It involves neurosurgical implantation of electrodes into specific deep brain structures — most commonly the subcallosal cingulate cortex (area 25) or the nucleus accumbens — connected to a programmable pulse generator implanted in the chest.
DBS is investigational for psychiatric conditions in most settings and typically considered only for severe, chronic, treatment-resistant cases where all other options have been exhausted.
The evidence for DBS in depression is promising but still evolving. It is not a mainstream clinical option and should only be discussed in the context of specialized academic medical centers with significant neuromodulation expertise.
Emerging and Experimental Therapies
Several newer approaches are expanding the brain stimulation landscape:
- Theta Burst Stimulation (TBS) — an accelerated form of TMS that delivers the same therapeutic effect in three minutes rather than 37; FDA-cleared and increasingly used as a faster alternative to standard rTMS
- Magnetic Seizure Therapy (MST) — induces therapeutic seizures using magnetic rather than electrical stimulation, aiming to preserve ECT’s efficacy while reducing memory side effects; still investigational
- Transcranial Direct Current Stimulation (tDCS) — uses low-level electrical current to modulate cortical excitability; non-invasive and inexpensive, but evidence for depression remains mixed, and it is not yet FDA-approved for psychiatric indications
- Accelerated TMS (SAINT protocol) — multiple TMS sessions per day over a condensed week-long course; early results show rapid response rates in treatment-resistant depression
Comparing TMS, ECT, and Other Methods
| TMS | ECT | VNS | DBS | |
| Invasiveness | Non-invasive | Non-invasive (requires anesthesia) | Surgical implant | Neurosurgery |
| Anesthesia required | No | Yes | Yes (implantation) | Yes (surgery) |
| FDA-approved for depression | Yes | Yes | Yes | No (investigational) |
| Response rate (TRD) | 50–60% | 58–70% | Slower onset | Variable |
| Primary side effects | Mild headache, scalp discomfort | Memory disruption, confusion | Hoarseness, cough | Surgical risks, infection |
| Recovery time per session | None | 1–2 hours | N/A (device) | Weeks post-surgery |
| Setting | Outpatient clinic | Hospital/clinic | Surgical suite | Neurosurgical center |
Effectiveness
ECT produces the highest short-term response rates for severe, treatment-resistant depression. TMS is meaningfully effective — and for a broader population of patients, including those with moderate rather than severe depression.
A 2025 meta-analysis published in JAMA (PubMed) analyzing 34 randomized controlled trials found TMS significantly reduced depression severity with a large effect size (SMD = −1.55), with high-frequency rTMS showing the strongest results (SMD = −1.90). Brain stimulation therapy for depression and brain stimulation therapy for anxiety consistently show better outcomes when treatment is tailored to the individual’s specific presentation.
Safety and Side Effects
TMS carries the most favorable safety profile of any brain stimulation approach. Adverse effects are primarily mild and transient — scalp discomfort and headache during or shortly after sessions are the most commonly reported.
Invasiveness
TMS and tDCS are fully non-invasive — no surgery, no anesthesia, no implanted hardware. ECT is non-invasive in the sense that no devices are implanted, but it requires general anesthesia, which carries its own risk profile. VNS and DBS involve surgical procedures with all associated considerations.
Cost and Accessibility
TMS is covered by most major insurers for FDA-approved indications and is delivered in outpatient clinic settings. ECT is typically hospital-based and, while covered by insurance, requires more intensive logistical planning. VNS and DBS coverage varies considerably, and access is limited to specialized centers.
Recovery Time
TMS requires no recovery time — patients return to normal activity immediately after each session. ECT typically requires one to two hours of recovery per session due to anesthesia, and some patients experience confusion or fatigue that extends into the afternoon. Surgical approaches carry a multi-week recovery from the implantation procedure itself.
Frequently Asked Questions (FAQ)
What is brain stimulation therapy used for?
Brain stimulation therapy is used primarily for depression — including treatment-resistant cases — as well as OCD, anxiety disorders, PTSD, and, in investigational contexts, conditions like Alzheimer’s and addiction. Different methods have different FDA-approved indications.
Is brain stimulation therapy for depression effective?
Yes, across multiple methods. TMS produces meaningful improvement in up to 83% of patients in real-world settings. ECT has response rates of 58–70% in treatment-resistant depression. Both significantly outperform placebo in clinical trials.
How does TMS compare to ECT?
ECT generally produces higher short-term response rates in the most severe cases. TMS is preferable for most patients because it requires no anesthesia, no hospital setting, no recovery time, and carries a significantly milder side effect profile. The choice depends on severity, urgency, and patient preference.
Can brain stimulation therapy be used for anxiety?
TMS has demonstrated effectiveness for anxiety disorders, including GAD and OCD, and is FDA-approved for OCD. TMS for anxiety at LifeQuality TMS is available as part of a comprehensive outpatient treatment plan.
How do I know which brain stimulation therapy is right for me?
The decision depends on diagnosis, symptom severity, treatment history, and individual circumstances. A clinical evaluation with a qualified provider is the appropriate starting point. For those whose depression hasn’t responded to medication or therapy, TMS is typically the first brain stimulation option to explore given its accessibility, safety, and evidence base.
Finding the Right Brain Stimulation Approach for Your Situation
Brain stimulation therapy is not a single treatment — it is a category of approaches with meaningfully different mechanisms, risk profiles, and clinical applications. TMS offers the strongest combination of evidence, accessibility, and tolerability for most patients. ECT remains the most effective option for acute, severe cases where rapid response is essential. Newer approaches are expanding the possibilities for those who need them.
If you’re exploring whether TMS fits your situation, contact LifeQuality TMS in Brooklyn to speak with a specialist.