ADHD is one of the most prevalent neurodevelopmental conditions worldwide, affecting both children and adults across every demographic. The core symptoms—persistent inattention, impulsivity, and difficulty regulating behavior—don’t just affect performance in school or at work. They strain relationships, erode self-esteem, and disrupt daily routines in ways that ripple through entire families.
Stimulant medications like methylphenidate and amphetamines remain the most studied first-line option, and for many people, they work well. But medication doesn’t work for everyone.
The good news: a growing body of research confirms that effective alternative treatments for ADHD exist—and that the strongest outcomes often come from combining multiple approaches into a coherent plan.
What Are Alternative Treatments for ADHD?
“Alternative” in this context doesn’t mean unproven or fringe. It refers to evidence-supported, non-pharmacological interventions that address ADHD symptoms through behavioral, lifestyle, brain-based, or nutritional pathways. Some work best as standalone strategies; most are most effective when integrated with one another or used alongside medication under professional guidance.
The categories worth understanding are:
- Behavioral and psychological therapies
- Lifestyle-based approaches (diet, exercise, sleep)
- Brain-based interventions such as TMS and neurofeedback
- Supplements and nutritional support
- Behavioral and Psychological Therapies
Cognitive Behavioral Therapy (CBT)
CBT has the strongest evidence base of any non-pharmacological intervention for adult ADHD. A 2025 meta-analysis in Frontiers in Psychiatry confirmed that behavioral and cognitive interventions produce meaningful improvements in ADHD symptoms and functional outcomes—particularly for adults, an area where medication alone often falls short.
The approach targets the thinking patterns and behavioral habits that fuel inattention and avoidance, including procrastination, poor time management, and emotional dysregulation.
For those already working with a mental health provider, LifeQuality TMS’s patient resources explain how brain-based treatments can work alongside therapy as part of a wider treatment plan.
Sessions typically address:
- Breaking tasks into manageable steps and creating consistent routines
- Identifying and interrupting the avoidance cycle that derails follow-through
- Building emotional regulation skills to reduce impulsive reactions
- Developing organizational systems that lower the cognitive burden of daily life
Unlike medication, CBT’s gains tend to persist after the formal intervention ends. That durability is one of its most clinically meaningful advantages.
ADHD Coaching
ADHD coaching operates differently from therapy—it’s less focused on psychological patterns and more on practical, day-to-day execution. A coach helps individuals set concrete goals, build accountability structures, and develop the external scaffolding that many ADHD brains genuinely need to function well. It’s not a treatment in the clinical sense, but for adults managing work and personal responsibilities, it often bridges the gap between knowing what to do and actually doing it.
Mindfulness-Based Interventions
Mindfulness training addresses one of the most overlooked deficits in ADHD: metacognitive awareness, or the ability to notice when attention has drifted and redirect it without self-judgment.
A 2024 comparative review published in the Journal of Affective Disorders evaluated neurofeedback, tDCS, and rTMS as non-pharmacological approaches for adult ADHD, noting that medication showed little to no effect in several reviewed studies — reinforcing the case for non-drug pathways. Mindfulness-based interventions complement these approaches by building the internal regulation skills that technology-based treatments cannot directly teach.

Lifestyle-Based ADHD Alternative Treatments
Nutrition and Diet
Nutritional interventions occupy a complex corner of the ADHD research landscape. The evidence varies considerably by approach. Omega-3 fatty acid supplementation has the most consistent support—multiple systematic reviews have found reductions in ADHD symptoms, particularly in individuals with lower baseline levels. The effect size is modest, but the risk is essentially zero, making it a reasonable adjunct for most people.
Artificial food color elimination has shown measurable, if limited, benefits in children who are sensitive to these additives. More restrictive elimination diets have produced results in some studies, but they are demanding to sustain and work best when guided by a clinician who has identified specific food sensitivities.
| Nutritional Approach | Evidence Level | Best Suited For |
| Omega-3 supplementation | Moderate | Children and adults with low omega-3 intake |
| Artificial color elimination | Moderate | Children with identified color sensitivity |
| Restricted elimination diets | Low–Moderate | Those with identified food triggers |
| Zinc supplementation | Low | Zinc-deficient individuals |
| Iron supplementation | Low | Iron-deficient children |
| Sugar restriction | Insufficient | Not well-supported by current evidence |
Exercise and Physical Activity
Aerobic exercise is among the most underutilized adhd alternative treatments available. It increases dopamine and norepinephrine levels in the prefrontal cortex—the same neurotransmitter pathways targeted by stimulant medication—which helps explain its reliable attention-boosting effects. Even a single session of moderate exercise produces measurable improvements in executive function. Regular practice deepens those gains.
What works best:
- 20–30 minutes of moderate aerobic activity, at least 4–5 times per week
- Timing exercise earlier in the day to capture the subsequent attention window
- Activities with built-in social or competitive engagement, which tend to hold interest more reliably for ADHD brains
Sleep Optimization
Sleep disruption is far more common in ADHD than is often recognized, and it creates a feedback loop that worsens core symptoms. Poor sleep degrades the exact cognitive functions already compromised by ADHD—sustained attention, impulse control, and working memory.
Addressing sleep hygiene isn’t a glamorous intervention, but in clinical practice, it frequently produces meaningful symptom relief that no supplement can replicate. Consistent sleep and wake times, screen-free wind-down periods, and managing stimulant timing to avoid late-day interference are all worth prioritizing.
For those whose sleep difficulties are entangled with anxiety or low mood, therapy for anxiety may address the underlying drivers rather than just the downstream sleep disruption.
Brain-Based Alternative Treatments
TMS Therapy for ADHD
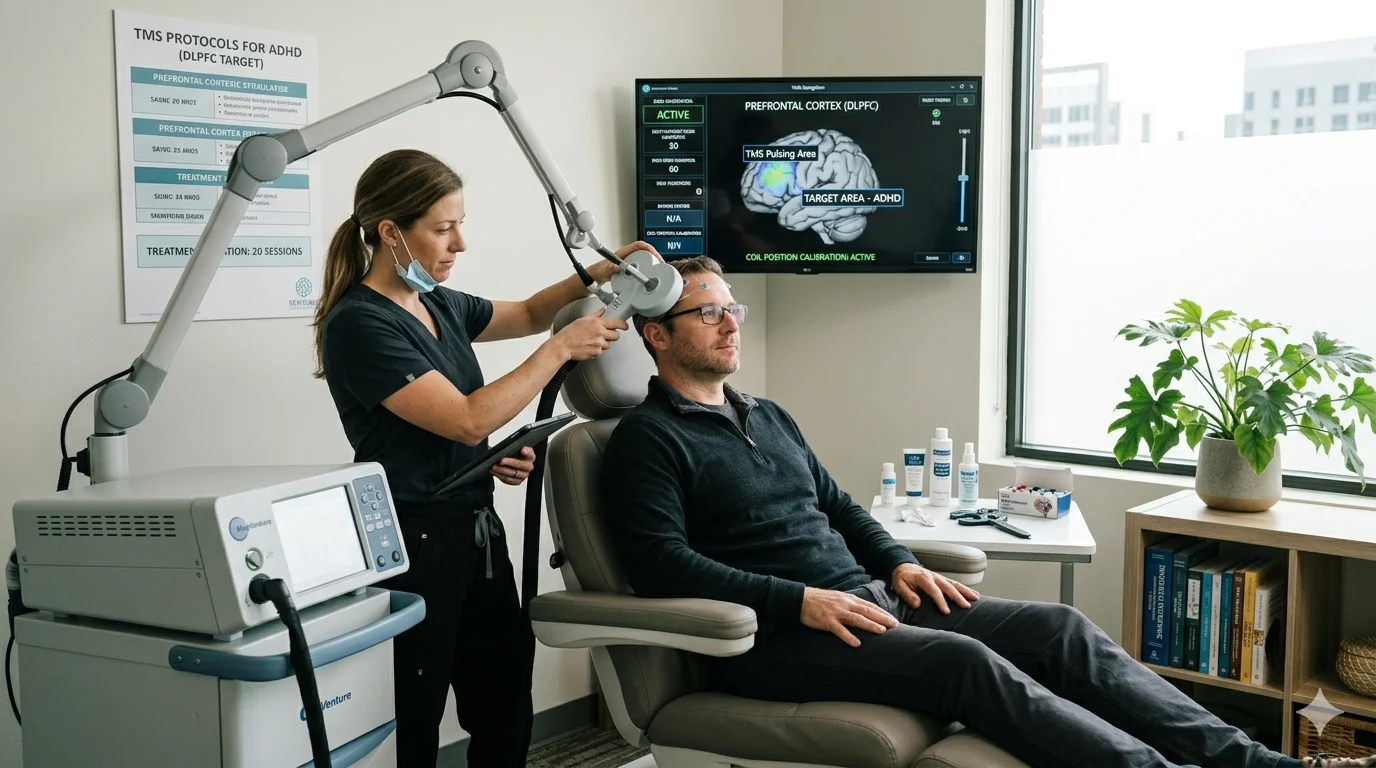
Transcranial Magnetic Stimulation (TMS) is one of the most promising and actively researched adhd alternative treatments in the current clinical landscape. TMS uses focused magnetic pulses to stimulate specific brain regions—particularly the right dorsolateral prefrontal cortex, an area consistently associated with attention regulation and impulse control in ADHD.
The research findings are noteworthy. A 2025 systematic review and meta-analysis published in Brain and Behavior (PMC) analyzed eight randomized controlled trials involving 325 ADHD patients and found that TMS significantly improved inattention (SMD = −0.94, p < 0.001) and hyperactivity/impulsivity (SMD = −0.98, p < 0.001) compared to non-TMS interventions over 3–6 weeks. Crucially, improvements in inattention symptoms persisted at one-month follow-up, suggesting that TMS produces durable neurological changes rather than temporary symptom masking.
TMS is FDA-approved for treatment-resistant depression and OCD. LifeQuality TMS in Brooklyn uses the BrainsWay deep TMS device, which reaches deeper cortical areas than traditional TMS coils—a distinction that may matter for ADHD, where deeper prefrontal circuits are involved. You can learn more about what TMS treatment involves before booking a consultation.
Neurofeedback
Neurofeedback uses real-time brainwave monitoring to teach individuals how to self-regulate neural activity patterns associated with attention and impulse control. Sessions are non-invasive and don’t involve medication. The research evidence is moderately supportive, particularly for younger children, though results vary significantly between individual,s and study quality across the field remains uneven.
Neurofeedback’s strongest case is as a complementary tool within a broader treatment plan. It’s time-intensive and can be costly, so it’s worth having realistic expectations about what it can and cannot achieve when used alone.
Supplements and Natural Support Options
Beyond omega-3s, several other nutritional supplements have been studied in ADHD populations. The evidence is largely preliminary but worth knowing:
- Magnesium: Some research links ADHD symptoms to magnesium deficiency; supplementation may help in deficient individuals
- Vitamin D: Low levels are more common in children with ADHD; repleting deficiency appears to support general cognitive function
- Zinc: Has shown modest symptom reductions in zinc-deficient children, particularly for hyperactivity
- Iron: Iron deficiency, even without anemia, correlates with ADHD severity in some studies; supplementation should be medically supervised
None of these is a substitute for evidence-based treatment. They are low-risk additions that may support the broader plan—especially when deficiencies are confirmed through testing.

Combining Treatments for Maximum Effectiveness
ADHD management is not one-size-fits-all, and no single alternative adhd treatment delivers comprehensive results in isolation. The most meaningful, lasting improvements tend to come from layering complementary approaches in a coordinated plan.
A well-structured non-medication strategy typically includes:
- Behavioral therapy as the clinical backbone—CBT for adults, parent training for families of younger children
- Regular aerobic exercise to support prefrontal dopamine regulation daily
- Nutritional optimization—particularly omega-3 supplementation and, where relevant, dietary adjustments
- Brain-based intervention, such as TMS or neurofeedback, for targeted neurological support
- Sleep hygiene protocols to prevent the compounding effect of sleep disruption on core ADHD symptoms
For individuals whose ADHD overlaps with depression—a common pairing—exploring TMS for depression may address both conditions through the same non-invasive treatment pathway.
Frequently Asked Questions
Can alternative treatments fully replace ADHD medication?
For individuals with mild symptoms, non-medication approaches may be sufficient. For most, they work best as complements to medication rather than complete replacements. Any changes to a treatment plan should be made with a qualified provider.
Which alternative ADHD treatment has the strongest clinical evidence?
Behavioral therapy—particularly CBT for adults and parent training in behavior management for children—has the most consistent evidence base. TMS is emerging as a strong option for those who need neurological-level intervention.
Is TMS safe for ADHD?
Research to date reports only minor adverse events with TMS for ADHD, primarily mild headache and temporary scalp discomfort. No serious adverse events have been documented in clinical trials. TMS is already FDA-approved for depression and OCD.
How long does it take to see results from non-medication ADHD treatments?
CBT typically shows meaningful results within 8–12 weeks of consistent engagement. Exercise produces short-term cognitive benefits within days, though lasting gains require ongoing commitment. TMS results vary by individual; a qualified provider can give realistic expectations based on a clinical assessment.
Who is a good candidate for TMS as an ADHD alternative treatment?
TMS is particularly relevant for individuals who haven’t responded adequately to medication, who experience intolerable side effects from stimulants, or who prefer a non-drug neurological intervention. Older adolescents and adults are the primary populations in current research. A clinical evaluation with a TMS provider is the appropriate first step.
Taking the Next Step Toward Non-Medication ADHD Care
ADHD is highly treatable, and the path forward doesn’t have to run exclusively through a prescription. If you’re considering TMS as part of a non-medication approach, contact LifeQuality TMS in Brooklyn to speak with a specialist about whether it’s the right fit for your situation.